How To Write A Good SOAP Note
A simple guide on How To Write A Good SOAP Note.
What is a SOAP Note? Also called SOAPI note
A SOAP note is a document that contains detailed information about the patient. It is usually written in an organized manner with clearly 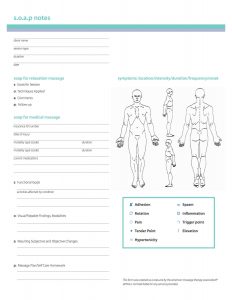 identified components. Healthcare professionals use a SOAP note to document their patients’ medical histories as part of their medical records. A SOAP note provides a standard format that clinicians can use to present patients’ information in an organized manner. The document allows an easy review of client documents. The acronym “SOAP” has been generated based on the specific components of the document.
identified components. Healthcare professionals use a SOAP note to document their patients’ medical histories as part of their medical records. A SOAP note provides a standard format that clinicians can use to present patients’ information in an organized manner. The document allows an easy review of client documents. The acronym “SOAP” has been generated based on the specific components of the document.
SOAP or SOAPI Note comprises five sections namely
the subjective data, objective data, assessment, plan, and Intervention. Each section contains different types of information.
Do you need SOAP Note Writing Help?
S: Subjective
The subjective section contains information that has verbally been presented by the patient concerning his or her illness. Under this section, the clinician gathers information about the onset of the current illness, the location of pain, the type of pain, alleviating factors, the main source of the pain, and the patterns of associated symptoms.
O: Objective
The objective section contains information that has been collected after the clinician has made an objective observation of the client. The information is considered objective because it comprises factors that can be seen, heard, or measured. Under this section, the practitioner usually documents the vital signs such as changes in body temperature, physical exam results, as well as the outcomes of diagnostic tests.
A: Assessment
The other part of a SOAP note is the assessment section. Under this section, the clinician documents the differential diagnosis as well as the primary diagnosis of the patient’s condition.
P: Plan
The plan refers to the patient’s plan of care.
In this segment, the clinician outlines the specific interventions that will be implemented to address the patient’s problem. It may include additional tests that should be performed and the treatment options that should be prescribed and administered.
I: Intervention
Interventions are the things we perform for the patient. Treatments, drugs, and instructions offered to the patient throughout your shift are examples of interventions. Check out a sample soap note.
Count on Top Nursing Papers.com with your How To Write A Good SOAP Note Task
The nurse should know how to write a good SOAP note that can be used to gain insight into the patient’s problem. A SOAP note must contain four headings written Subjective, Objective, Assessment, and Plan. The specific types of information that are to be included under this section include the Chief Complaint, History of Present Illness, the Patient’s Medical History, Review of Systems, as well as Current Medications and Allergies. As earlier mentioned, the specific details that are to be written under the objective section include; vital signs, laboratory data, physical exam findings, and imaging results. When documenting the assessment section, the clinician should synthesize the subjective and objective data and utilize it to summarize the patient’s case. He or she should write differential diagnoses of the patient’s condition in order of importance. The primary diagnosis should then be selected from the list. The plan section should be written clearly and concisely to help other clinicians understand what should be done next to address the patient’s problem. It should detail the specific tests required and their rationale, the therapy required, referrals, and an outline for patient education. Let us write a nursing note now.
Order a Well Written SOAP Note at Top Nursing Papers.com
With a well-written SOAP note, the clinician can easily understand the patient’s problem and establish the primary diagnosis based on subjective and objective data. The clinician must be careful to maintain a high level of accuracy when writing a SOAP note. The reason is that the documentation of inaccurate data may harm the patient. Generally, a SOAP note is advantageous for healthcare professionals because it helps them to document the patient’s information in an organized manner that can easily inform a clinical decision.
Do you need writing help on How To Write A Good SOAP Note paper? Ask the experts. Help With SOAP Note Paper
Popular SOAP Note topics we can help on;
Make a SOAP Note: Assessing Ear, Nose, and Throat
Make a SOAP Note: Assessing the Heart, Lungs, and Peripheral Vascular System
Episodic SOAP Note
Creating Case Notes MENTAL HEALTH COUNSELING
Participant Observation: A Study in Gender Roles
Differential Diagnosis for Skin Conditions
Looking for Focused soap note and patient case presentation writing help? We are the ultimate SOAP NOTE nursing writers. Order a custom paper now.
Get the solution to How To Write A Good SOAP Note assignment from the experts!
Get real answers to these and more nursing questions;
What is included in a SOAP note?
What are the 4 defined sections on a SOAP note? or What are the 4 headings of a SOAP Note?
How are SOAP notes organized?
What are the types of SOAP Notes? Check out types of therapy notes
